Oral and Maxillofacial Surgeon in London
If you're looking for one of the best maxillofacial or oral surgeons in London, then our welcoming and state-of-the-art Hampstead oral surgery can help.
Our specialist Consultant Oral Surgeon, Mr. Anish Shah (GDC Specialist No: 76559), has over 24 years experience, is a renowned expert in his dental field and takes pride in being an extremely gentle yet highly effective surgeon.
Patients in Hampstead and across London have been choosing Dental Perfection for their oral and maxillofacial surgery procedures since 1979.
Choose our oral surgery treatment and benefit from:
- Highly skilled and specialist oral surgeon (24+ years experience)
- Sedation options
- Experts in helping nervous patients
- Long established practice in North London since 1979
- Less than a minute’s walk from Hampstead Underground Station
- Rated 5* via patients on Google Business
See inside our state-of-the-art London oral surgery clinic





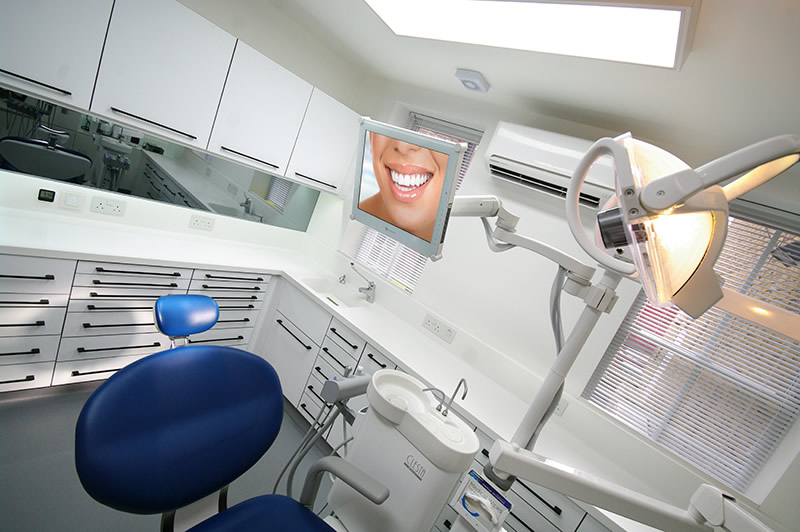
Take a tour of our state-of-the-art clinic in Hampstead
What is oral surgery?
Oral Surgery involves the diagnosis, management and sometimes surgical or medical treatment of conditions of the mouth and the adjacent and surrounding structures. Oral Surgery is closely related to Oral & Maxillofacial Surgery/Medicine.
Some of the oral surgery treatments we perform at our North London practice here in Hampstead include:
| Surgical removal of impacted/buried teeth | |
| Surgical removal complicated buried roots | |
| Coronectomy | |
| Surgical Endodontics/Apicectomy | |
| Surgical Orthodontics/Exposure of teeth | |
| Enucleation of cysts of jaw | |
| Biopsy/Excision of lesion of mouth including lips, tongue, palate | |
| Pre-prosthetic surgery including vestibuloplasty | |
| Closure/repair of pro-antral fistulae +/- pedicled fat graft | |
| Removal of stone/calculus from salivary gland duct | |
| Biopsy of minor salivary gland (labial gland biopsy) | |
| Ankylotomy (tongue tie release) |
Our oral surgeon also covers other issues, such as:
| Diagnosis and treatment of facial pain | |
| Oral medicine | |
| Recurrent oral aphthous ulcers | |
| Red/white patches of the mouth | |
| Burning mouth | |
| Dry mouth | |
| Hyper-salivation | |
| Lumps and bumps of the mouth | |
| Use of muscle relaxing injections for the treatment of TMJ related conditions, gummy smiles | |
| Oral manifestations of systemic disease |

Your specialist London Oral Surgeon
If you’re ready for expert oral surgery from a friendly and highly experienced dentist, our specialist oral surgeon, Anish Shah (GDC Specialist No: 76559), can help.
Mr Shah has over 20 years experience, is a renowned expert in his dental field and takes pride in being an extremely gentle yet highly effective surgeon.

Oral surgery review via Google Business
"Dear Dr. Sanei and Dr. Rahbaran - you are the best dentists in the world! You have converted me completely from hating going to see the dentist to looking forward to it!! That's just beyond magic. You have explained every single procedure during the surgery and treatment I felt so well looked after in your clinic.
Your skills and knowledge is fantastic. I cannot thank you both enough. I recommend you to every family member of mine and please keep on doing what you do - it is a truly life changing experience :)
I would also like to thank Debra and Stephanie and Lisa you ladies are so awesome and it's a pleasure to be your patient!! I cannot recommend this clinic enough!"
![]()
Bailu Lu
Oral surgery treatments explained:
-
Not all wisdom teeth need to be removed. However, in some cases, the arrival of these teeth can cause serious problems, resulting in pain, swelling, or infection. Read more about wisdom teeth removal or the costs of wisdom teeth removal.
-
Developing an infection in an inner tooth can be extremely painful. Fortunately, for the highly skilled endodontics team at Dental Perfection, root canal surgery is an everyday, routine procedure. Read more about root canal surgery.
-
Whilst removing a tooth may seem like a simple process, certain issues can make the procedure more complicated. This means the extraction procedure may need to be altered. Read more about tooth extractions.
-
If you were to have your tooth extracted by an oral surgeon, the root would be surgically removed with the rest of the tooth. However, if you were to lose a tooth through trauma or decay, it is possible that the roots may be left behind.
When a root is retained by the jawbone and gums without the crown present, it can cause a wide range of problems. Mouth infections and severe pain are extremely common and this is why the surgical removal of these buried roots is necessary.
Whilst some retained roots will only require a simple, straightforward extraction under local anaesthetic, others may require lengthier oral surgery procedures.
In particularly difficult retained root extractions, it is possible that a small section of the gum or jawbone may need to be removed in order to retrieve the root. For these procedures, your oral surgeon will use a general anaesthetic, so you won’t feel a thing.
-
Jaw cysts are little sack-like pouches that form in the tissues of the jaw and fill with fluid. They are generally benign, tend to grow very slowly, and do not present any noticeable symptoms.
They can arise from infections or trauma and are most common in adults. Depending on the location, type and size of the cyst, your oral and maxillofacial surgeon may want to remove the cyst to let your jaw tissues repair themselves and to prevent another cyst from forming.
If a cyst is aggressive and growing, you may need to consider maxillofacial surgery.
-
Sores on the tongue, lips, inner cheek and mouth are most often caused by minor viral infections or injuries. Whilst they can sometimes be painful or embarrassing when visible, they rarely require immediate medical attention.
However, in some cases, oral lesions can be a symptom of mouth cancer, so it is possible you may be sent for a biopsy. If you have particularly painful or recurrent lesions in or around your mouth, your dentist may recommend a biopsy by an oral and maxillofacial surgeon.
This is a simple process whereby a small tissue sample of the lesion will be removed then sent away to a laboratory for testing. This will be carried out under local anesthesia.
Once the results are back, your oral surgeon will call you back into the office where you may decide to have the lesion removed entirely.
-
Ulcers in the mouth are one of the most common oral conditions we see and, more often than not, they usually clear up on their own within a week or two. Although they are mostly harmless, it is always worthwhile speaking to your oral and maxillofacial surgeon about the possible causes of your mouth ulcers.
If a mouth ulcer keeps coming back, it may be due to certain vitamin deficiencies, immune conditions, infections, or a syndrome.
It is likely that your oral surgeon will suggest a blood test to diagnose the cause, which they may then be able to treat. When an ulcer becomes more painful and red, it can be a sign of an infection, so make sure you visit your dentist or GP as soon as possible.
However, if you have had a mouth ulcer for more than three weeks, it is essential that you visit your Oral Surgeon urgently. Whilst most mouth ulcers are nothing to worry about, a long-lasting ulcer can be a sign of mouth cancer, so it is always best to get it checked early.
-
Dehydration and stress are common causes of temporary mouth dryness but, if it persists, it is possible you may have xerostomia.
This can cause extreme difficulty when eating, causing problems with tasting, chewing and swallowing. Dry mouth can be a side effect of certain medications, especially heart, blood pressure, and depression pills.
A dry mouth also creates the ideal conditions for tooth decay, since there is no barrier to keep acids and bacteria at bay. You must make sure you visit your oral surgeon if you have this condition, as you’re at much higher risk of developing tooth decay or gum disease.
-
Whilst some foods may make your mouth water, excess saliva can be problem that is difficult to live with.
Many assume excess saliva is caused by overproduction however it could be down to a wide range of other issues such as acid reflux, side effects of medication, infection or inflammation in the gums, badly-fitting dentures, or even a sinus infection.
If excess saliva persists, it is always wise to visit your oral surgeon for consultation.
-
BMS, or burning mouth syndrome, is a condition described by some patients as feeling like their mouth has been scalded, however other symptoms include a constant bitter taste or a generally sore mouth.
More common in women than men, this condition can cause extreme discomfort so it is important that you contact your dentist if you believe you may be experiencing BMS. Whilst a diagnosis cannot be reached through laboratory tests, your oral surgeon may recommend a blood test to find the potential cause.
Many other conditions have been said to contribute to BMS, such as nutritional deficiencies, menopause, dry mouth, diabetes, fungal infections, acid reflux and even depression and anxiety. Treatment for burning mouth syndrome may include a combination of medication, nutritional supplements, diet modifications and rehydration.
-
Lichen planus is an inflammatory condition that can affect many different areas of the body, including your skin and oral cavity; presenting as white lacy patterns, a mixture of red and white patches on the inside of the cheeks, or open sores.
The lesions of oral lichen planus may cause sensitivity to certain foods or brushing, tenderness or burning sensations, or pain. If you believe you may have this condition, it is extremely important that you obtain a correct diagnosis.
This is something your oral surgeon can help you with, as they will be able to carry out a small biopsy to confirm the condition. Whilst we know it is non-infectious, the actual cause of this issue is currently unknown.
It is said that oral lichen planus affects around one to two per cent of the population around the world. In most cases, oral lichen planus cannot be cured, however it has been known to go away on its own.
In some cases, oral lichen planus can persist for a number of years. If you are experiencing pain as a result of the lesions, this can be treated using topical ointments, steroids, and other drugs.
-
This is a general term referring to any kind of pain felt in the mouth, jaws and the face. A common symptom of other conditions or illnesses, an estimated 95% or orofacial pain comes as a result of dental causes.
Because of this, orofacial pain is a key concern for maxillofacial and oral surgeons.
Your North London oral surgery team in Hampstead
No matter what type of oral surgery you may need, our expert dental team will do everything they can to ensure you are happy at every stage of the process.
If you have any questions you would like to ask our oral surgeon about your procedure, or would like to find out what course of treatment might work for you, book your oral surgery consultation by calling us on 020 7431 2710, or come and see us at our Hampstead surgery.
We have been working with clients from all over North London (including St Johns Wood, Belsize Park, Highgate, and Swiss Cottage) from our Hampstead clinic since 1979.
Our state-of-the-art clinic is less than a minute's walk away from Hampstead Underground Station.
Extra help about oral surgery
Patient satisfaction is very important to us
